Sygeplejersken
Oxygen therapy: The effect and discomfort from two types of catheter
The two oxygen catheters tested are basically equally effective in terms of the oxygen saturation of patients, but the binasal catheter causes less discomfort than the oxygen catheter with a foam rubber plug. The study concludes that nurses could be more aware of the type of catheter used for oxygen therapy, and argues for increased use of the more comfortable binasal catheters.
Sygeplejersken 2000 nr. 10, s. 46-49
Af:
Karen Bidstrup, sygeplejerske, cand.pæd.psyk.,
Birthe D. Pedersen, lektor, ph.d., cand.cur.,
Jytte Astrup, social- og sundhedsassistent,
Anette Nørby Dahl, sygeplejerske,
Tove Svendsen, sygeplejerske,
Susanne Lundager Toft, sygeplejerske

The purpose of the study has been to study two types of oxygen catheters, the binasal catheter and the oxygen catheter with a foam rubber plug, and compare them in terms of the discomfort experienced by the patient and the effect of oxygen therapy.
Design: prospective, non-blind, randomised, consecutive comparative study of two patient groups treated with different types of oxygen catheter. Data has been collected partly by observation, partly by asking questions and partly by measuring oxygen saturation in the blood. The study was carried out on the recovery ward of the Department of Anaesthesiology, Århus County Hospital/Århus University Hospital.
Subjects: 70 patients aged between 20 and 50 took part in the study. All had undergone minor surgery under general anaesthetic, for example, cruciate ligament reconstruction, fracture repositioning, removal of osteosynthetic material, hysterectomy, hysteroscopy and varicose vein operations. The patients had healthy hearts and lungs, they were not overweight nor did they suffer from plastic allergy. 30 patients underwent oxygen therapy using binasal catheters and 40 patients using foam rubber catheters. Effect measurements: feelings of discomfort based on observations and questions (frequency type), effect of the oxygen therapy via recording of transcutaneous oxygen saturation (pulse oximetry).
Results: The oxygen saturation level was the same for patients with foam rubber catheters and binasal catheters. The discomfort experienced was greater (P<0.05) when using foam rubber catheters (22/40) than when using binasal catheters (9/30). Altogether, 23 attempts to remove the foam rubber catheters were recorded compared with only 3 attempts to remove the binasal catheters. With treatment using foam rubber catheters discomfort was experienced much more frequently than with the binasal catheters (dry nose: 30 percent as opposed to 3 percent, P<0.05); blocked nose: 25 percent as opposed to 3 percent, P<0.05). The number of smokers was equally divided between the two groups.
Conclusion: There is no significant difference in the effectiveness of oxygen therapy between binasal and foam rubber catheters. The discomfort experienced, such as a dry or blocked nose, occurred the least with the binasal catheter.
Introduction
After a general anaesthetic it is well-documented that postoperative hypoxia can occur if oxygen supplementation is not given (1,2,3). Even though patients are postoperatively given humidified oxygen, many of them report extreme discomfort with the postoperative oxygen therapy. The humidifying of oxygen is achieved through passing the oxygen through a coldwater humidifying system (Kendall bubble-humidifier) and is supplied to the patient through a nasal catheter with a foam rubber plug inserted into one of the nasal passages. Discomfort occurs in patients sleeping who repeatedly remove the oxygen catheter and subsequently expose themselves to the risk of postoperative hypoxia. When awake, patients often complain about an itchy, dry, sensitive or blocked nose. Furthermore, they complain of a bad smell, that their eyes water or that they feel an urge to sneeze, which can exacerbate pain caused by the surgical wound. One explanation for these forms of discomfort could be the oxygen catheter with foam rubber plug. A number of recovery wards across the country have begun to use
Side 47
the somewhat more expensive binasal catheters for oxygen therapy in the postoperative phase, in the belief that these catheters are more comfortable for the patients (4). A review of the literature has revealed that no studies exist to document this hypothesis. In contrast, a number of comparative studies of nasal catheters in comparison with face masks have been found showing a patient preference for the oxygen catheter (5,6). Another study reveals that patients experience less discomfort when humidified oxygen as opposed to unhumidified oxygen is channelled through a binasal catheter (7).
With the initiation of postoperative oxygen therapy on the recovery ward it is the nurse's responsibility and duty to minimise the amount of discomfort experienced by the patient and also to continuously ensure that the patient is supplied with sufficient oxygen.
The purpose of the study was therefore to compare the two methods of postoperative oxygen therapy, namely nasal catheters with foam rubber plugs and binasal catheters, from the perspective of both discomfort and the effectiveness of the oxygen therapy.

Material and methods
The study was designed as a consecutive, prospective, randomised non-blind study, where 71 patients were randomised into two groups, which were each treated with a different type of oxgyen catheter, oxygen catheters with foam rubber plugs or binasal catheters. The randomisation procedure was performed before the study was initiated and in this respect sealed envelopes with consecutive numbers were used. Under the prerequisite that the study had to demonstrate at least a 40 percent difference between the two types of therapy with 2 α = 5 (the test's significance level) and β = 10 percent (the test's strength = 100 minus β = 90 percent), each group had to contain 35 patients.
The study included both female and male patients aged between 20 and 50 who had been admitted for minor surgery. Patients suffering from any heart or lung disorders were excluded. The treatment was to be performed under general anaesthetic and the patients were to be under for no longer than three hours.
The following types of operation were included in the study: cruciate ligament reconstruction, repositioning of fracture, removal of osteosynthetic material, hysterectomy, hysteroscopy as well as varicose vein or hernia operations. Patients excluded from the study were those with heart and/or lung disorders requiring treatment, those allergic to plastic and those overweight. A further group excluded from the study were patients with chronic perioperative oxygenation problems (oxgyen saturation < 0.90) with a drop in their systolic blood pressure to 70 percent of the norm or below, and patients who had been under anaesthetic for longer than three hours.
Oxygen saturation was measured by pulse oximetry (SO2 0.93-0.98). The measurements were taken on arrival at the recovery ward and also after 15, 30, 45 and 60 minutes. All data regarding oxygen saturation was recorded on special charts.
Registering discomfort was done partly by observation and partly by putting questions to patients whose responses were then recorded on charts which contained the following categories of discomfort:
Sneezing, dry nose, bad smell, watery eyes, nasal pain, itchy nose, headache, blocked nose, etc. In addition, it was recorded that on many occasions patients attempted to remove the oxygen catheter, that is, physically remove the catheter from the nose. The recordings were made by the nursing staff partly based on the patient's spontaneous expression of their feelings and partly after an hour's therapy with the oxygen catheters as well as at the end of the therapy, that is, when the patient was returned to the main ward. At the end of the treatment the patients were asked if they had experienced any of the above forms of discomfort. They
Side 48
were also asked if they were smokers or non-smokers. The nursing staff who questioned the patients recorded the answers on a chart (Table 1).
The comparison of the groups in terms of oxygen saturation was performed using the Mann Whitney test corresponding to the five measurement times. Comparison of the group in terms how often patients felt discomfort was conducted using an x2-test (8).
Patients who met the inclusion criteria were contacted before the day of the operation. Treatment with the two types of oxygen catheters did not involve any risk, as patients were ensured a sufficient amount of oxygen with both types of catheter.
Results
All patients who met the inclusion criteria in the study period took part. Of the 71 patients who originally took part in the study only one withdrew. This was due to perioperative circulatory problems. The remaining 70 patients, male and female, with a mean age of 30, ranging from 20 to 50 years, underwent the following surgical treatments: cruciate ligament reconstruction, repositioning of fracture, removal of osteosynthetic material, hysterectomy, hysteroscopy and varicose vein operations. Randomisation meant that 40 patients were treated with catheters with foam rubber plugs and 30 patients with binasal catheters. There was an equal distribution in terms of age, gender and operation category in the two groups. The number of smokers was the same in each group. These were distributed in the following way: 18 out of 40 patients using the foam rubber catheter were smokers, which corresponds to 45 percent. In the group treated with binasal catheters 14 out of 30 were smokers, which corresponds to 47 percent. The randomisation process thus resulted, as anticipated, in the equal distribution of smokers in both groups.
The mean oxygen saturation in patients with foam rubber catheters and binasal catheters did not differ significantly at some of the observation times (Table 1). There was, however, a tendency for there to be a slightly lower oxygen saturation among patients with foam rubber catheters.
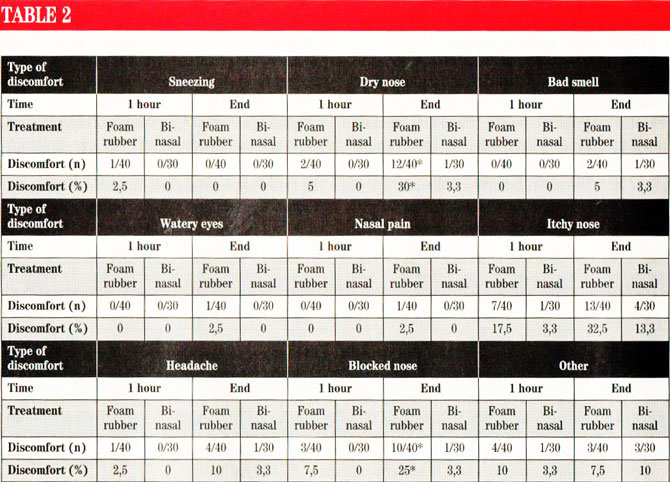
The feeling of a dry or blocked nose was significantly (P<0.05) more frequent with the use of catheters with foam rubber plugs than with binasal catheters at the end of the treatment (Table 2), but not after one hour. There was no significant difference in the frequency of discomfort in the form of sneezing, bad smell, watery eyes, nasal pain and headache between the two groups either after one hour or at the end of the treatment
Side 49
(Table 2). With regard to treatment with oxygen catheters with foam rubber plugs discomfort was recorded in 22 out of 40 patients (55 percent) compared to9 out of 30 patients treated with binasal catheters(30 percent), a difference which was significant (P<0.05).
In the observation period 23 attempts to remove the catheter with foam rubber plugs were recorded compared to only 3 attempts to remove the binasal catheter.
Discussion
The study has shown that the degree of discomfort is greater among patients who after the operation were treated with oxygen catheters with foam rubber plugs than among patients treated with binasal catheters. The most serious side-effects from the use of oxygen catheters with foam rubber plugs were the sense of a dry or blocked nose.
The study found no significant difference in the oxygen saturation among patients in the two groups. The mean saturation was, however, slightly lower for patients in the group with foam rubber catheters at all measurement times. This may be due to the fact that patients treated with foam rubber catheters very often removed or attempted to remove the catheter, which was not the case with the patients using binasal catheters. Under the category ''Other'' on the chart, nausea was recorded. This recording must be treated with some reservation because nausea cannot automatically be attributed to discomfort caused by the catheter but might be due to many other things, such as the effect of the anaesthetic, the air on the recovery ward, nervousness, etc.
This study is the first of its kind to directly compare the degree of discomfort experienced when using oxygen catheters with foam rubber plugs and binasal catheters in connection with postoperative oxygen therapy.
It can be concluded that both methods of treatment are effective in terms of delivering sufficient oxgyen therapy but that the oxgyen catheters with foam rubber plugs cause greater discomfort among patients than binasal catheters. In terms of nursing care, the study can help sharpen awareness about which type of catheter should be used in oxygen therapy and at the same time contribute to the argument in favour of using the more comfortable binasal oxygen catheters instead of the catheter with a foam rubber plug. In the study the subjects involved were relatively young and admitted for minor surgery, and therefore underwent a rather brief course of oxygen therapy. With oxygen therapy of longer duration even more consideration should be given to the choice of catheter, in order to avoid the uncomfortable side-effects which a catheter with a foam rubber plug can cause. The side-effects may well be a major but unnecessary contributing factor to the lack of well-being during the patient's illness, hospital stay and oxygen therapy.
References
The project has received funding from the Aarhus University Hospital Research Initiative as well as from the Danish Nurses Organisation. The scientific ethical committee for Aarhus County has approved the project.
Litterature
- Chiolero R, Revelly JP, Ravussin P. Early postoperative hypoxia. Agressologie 1992; 33: 32-4.
- Hoffman C, Nakamoto D, Okal R, Clohesy JM. Effect of transport time and Fi02 on Sp02 during transport from the OR to the PACU. Nurse Anaesth 1991; 2: 119-25.
- Brown LT, Purcell GJ, Traugott FM. Hypoxaemia during postoperative recovery using continuos pulse oximetry. Anaesth Intensive Care 1990; 39: 235-243.
- Jensen AG, Corydon L, Pedersen B. Bedre forebyggelse af iltmangel hos nyopererede. Sygeplejersken 1992; 31: 4-7.
- Nolan KK, Winyard JA, Goldhill DR. Comparison of nasal cannulae with face mask for oxygen administration to postoperative patients. Br J Anaesth 1993; 70, 440-2.
- Amar D, Brodman LE, Winikoff SA, Hollinger I. An alternative oxygen delivery system for infants and children in the post-anaesthesia care unit. Can J Anaesth. 1991; 38: 49-53.
- Andersen SS, Hansen L, Bøggild NB, Kummerfeldt I. En sammenligning af patientkomforten ved brug af tør kontra fugtet nasal ilttilskud. Centralsygehuset i Esbjerg Anæstesiologisk Afdeling, marts 1993.
- Armitage P, Berry G. Statistical Methods in Medical Reasearch, third edition. Oxford: Blackwell Scientific Publications; 1994.
